Thyroid hormones play a crucial role in the body’s metabolism, and in patients with diabetes thyroid dysfunction diseases are common. Type 1 diabetes mellitus can be treated with daily insulin injections, but this treatment is often accompanied by multiple complications.
Studies have shown, however, that mesenchymal stem cells (MSCs), having produced remarkable improvement in diabetic rat models, can differentiate into insulin-producing cells that could be used for treatment of diabetes mellitus. To evaluate effects of bone-marrow-derived stem cell transplantation on rats with induced diabetes mellitus by assessing their thyroid hormones, thyroid autoantibodies, and structural changes in thyroid gland sections before and after MSC transplantation, this study used 40 adult male albino rats: 10 for MSC isolation; 30 randomly divided into control, diabetic, and MSC-treated groups. In 20, diabetes mellitus was induced by streptozotocin injection. Of the diabetic group, 10 were treated with bone-marrow-derived stem cells. Histological studies (light, electron microscopy) of thyroid sections were observed; thyroid hormones, thyroid peroxidase, and thyroglobulin antibodies were measured in the serum.
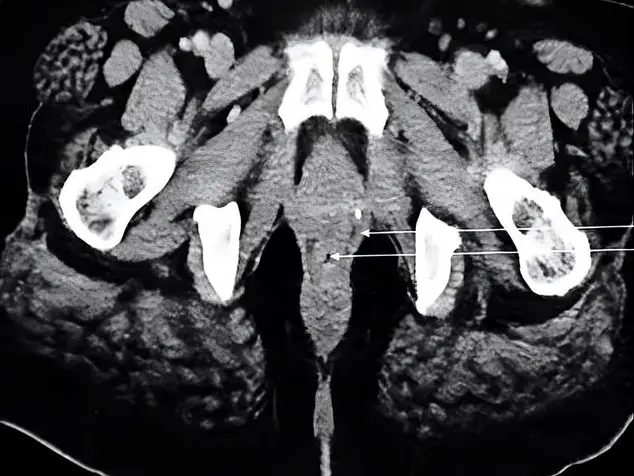
Diabetic rats’ thyroid glands showed distorted histological structure, a drop in thyroid stimulating hormone (TSH), and elevation of thyroid hormone level. Microscopically, the thyroid gland of bone-marrow-derived stem cell-treated rats yielded significantly ameliorated histological appearance and significantly increased TSH levels, along with thyroid hormones decreased toward normal levels. Diabetes induces thyroid dysfunction and thyroid tissue injury. Bone-marrow-derived stem-cell therapy protects against thyroid gland diabetes-induced tissue injury.