The present study was designed to assess the incidence of different anatomical variations of the left coronary artery (LCA) and their branches. Also, it was designed to study the dominance pattern of coronary arteries. It was carried out on 30 human adult cadaveric hearts, 200 three-dimensional coronary computed tomographic angiography (3D-CCTA) scans, and 200 coronary catheterization angiography obtained from the Anatomy, Radiology, and Cardiology Department, Beni-Suef, Cairo as well as El Minia University. The current work revealed that there was not any case of higher take-off origin of the left coronary artery. The incidence of the LCA branching mode was 74.1%, 24.18%, and 0.46% for the bifurcation, trifurcation, and tetrafurcation, respectively. A statistically significant correlation between the diagonal branches of the left anterior descending artery and the mode of branching of the LCA had been demonstrated. The incidence of coronary artery dominance was 77%, 14%, and 9% for right, left, and co-dominant pattern. It can be concluded that perfect knowledge of the anatomical variations of the mode of branching of the LCA is essential for cardiologists and radiologists, during diagnostic and therapeutic cardiac procedures.
Anatomical variations of the left coronary artery: a cadaveric and radiological study
Hanan D. Yassa1, Gaber H. Abdelfatah1, Nourhan T. Sabra1, Abd Elwakeel E. Essawy2
1 Department of Anatomy and Embryology, Faculty of Medicine, Beni-Suef University, Beni-Suef, Egypt
2 Department of Anatomy and Embryology, Faculty of Medicine, Cairo University, Cairo, Egypt
SUMMARY
Sign up or Login
List of abbreviations
CCTA: Coronary computed tomography angiography.
CT: Computed tomography.
CX: Circumflex artery.
D: Diagonal branch.
LAD: Left anterior descending artery.
LCA: Left coronary artery.
MB: Myocardial bridge.
OM: Obtuse marginal artery.
PDA: Posterior descending artery.
RCA: Right coronary artery.
RI: Ramus intermedius artery.
INTRODUCTION
Ischemic heart disease caused 7 million deaths all over the world in 2010, an increase of 35% since 1990 (Lozano, 2012). Whatever the etiology and pathophysiology of coronary artery disease are, the coronary artery remains the seat of the disease process. The increasing use of diagnostic and therapeutic interventional procedures necessitates that a sound basic knowledge of coronary artery pattern with dominance is essential (Das et al., 2010).
The anatomy of the coronary arteries has been described for at least three centuries. However, most of the reports are based on views and perspectives obtained from gross specimens (Fiss, 2007; Young et al., 2011).
The arterial supply of the heart is provided by the right and left coronary arteries. They are located between the epicardium and myocardium; these vessels arise from the bulbous aorta as two branches of the ascending aorta (Snell, 2011). The left main coronary artery originates from the left coronary sinus of Valsalva (Moore and Dalley, 2006). The morphology of the left coronary artery has been reported to present wide variability regarding its length, caliber, and mode of branching. Its trunk divides into several ways: bifurcation into left anterior descending (LAD) and circumflex (CX) branches, or trifurcation into LAD, CX, and median or ramus intermedius (RI) arteries (Beg et al., 2015). Tetra-and pentafurcation patterns of branching have been also mentioned (Reig and Petit, 2004; Roy et al., 2014). The bifurcation pattern has been described as the most frequent one (Chougule et al., 2014).
Recently, technical advances in computed tomography (CT) have improved image quality, diagnostic performance, and accuracy of coronary CT angiography (CCTA) (Graidis et al., 2015). Dose-reduction strategies have reduced radiation dose to an acceptable level, even lower than that from conventional coronary angiography (Altin et al., 2015). Three- dimensional CCTA is a noninvasive imaging modality, which can effectively show complex anatomy and variations of the coronary arteries (Erol et al., 2013).
Cardiac catheterization remains the gold standard in the diagnosis of coronary artery anomalies. The objective of angiocardiography is to establish the integrity and source of the coronary arteries (Takeuchi et al., 1979).
MATERIAL AND METHODS
Cadaveric Study
This descriptive study was done in 30 adult cadaveric hearts in the Department of Anatomy at Beni-Seuf, Cairo, and El Minia Universities of Medicine. The adult cadaveric hearts of both genders (aged 24-68 years) without any obvious pathology were included. The hearts with any gross pathology, traumatic damage, or congenital anomalies were excluded from the study. The heart was taken out by incising the fibrous pericardium and great vessels like aorta, pulmonary trunk, superior vena cava, inferior vena cava, and pulmonary veins. The specimens were collected, numbered, and preserved in a 10% formalin solution. The visceral pericardium and subepicardial fat were removed. The LCA and its branches were carefully dissected out and followed till their termination. The origin, course and termination of variations in varous branches, if any, were noted. To determine the dominant circulation, the origin of PIVA was noted in each specimen. Photographs of each specimen were taken using a digital camera, numbered, and labeled. The events followed were well-matched with the ethical standards for human experimentation. The ethical committee approved the study.
Radiological study
Coronary CT Angiography (CCTA):
Two hundred adult individuals of both genders (aged 24–68 years, free from major cardiac complaints and previous bypass surgery) were subjected to 3D-CCTA in certified radiology centers. Imaging was performed on 320-row CT scanners (Aquilion ONE, Toshiba Medical Systems, Tochigi-ken, Japan).
The main trunk of LCA was followed from its orifice until its division into the left anterior descending (LAD) and circumflex (CX) arteries. Its mode of branches was observed and recorded (Kini et al., 2007).
Coronary catheterization
(coronary angiogram):
Two hundred adult individuals of both sexes, free from major cardiac complaints, atherosclerotic lesions in coronary arteries, history of coronary stent insertion, and previous bypass surgery were subjected to coronary angiogram in the Cardiology Department at Beni-Suef University.
Statistical analysis
After compilation of collected data, an analysis was done using Statistical Package for Social Sciences (SPSS), version 20 (IBM, Chicago, USA).
Qualitative data were expressed as frequency and percentage. Chi-square test or Fisher’s exact test was used to examine the relation between qualitative variables. The differences were considered statistically significant when the p-value was <0.05.
RESULTS
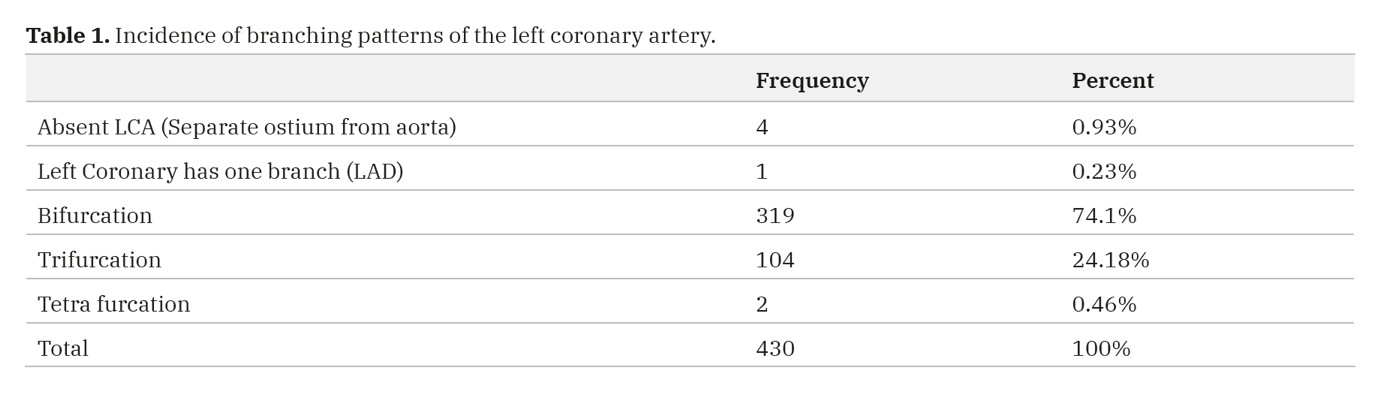
Out of 430 hearts (30 cadavers, 200 3D CT angiography, and 200 coronary catheterizations), the overall incidence of the different patterns of LCA branching mode was 0.23% in which LCA continues as LAD (one branch), 74.1% in bifurcation, 24.18% in trifurcation, and 0.46% in tetrafurcation patterns. And the incidence of absent LCA was 0.93% as LAD and LCX (Table 1) (Figs. 1,2,3).
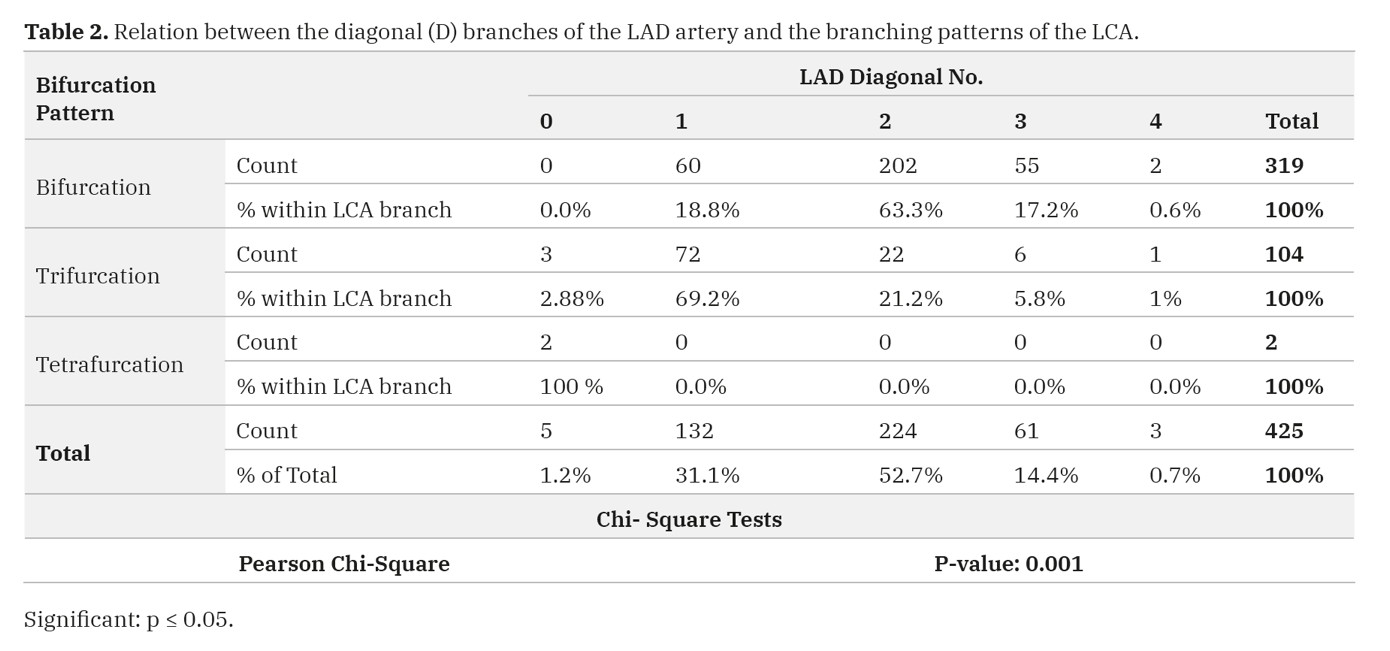
The diagonal (D) branches of the LAD artery were found in 319 hearts out of 319 with the bifurcation pattern (100%), 101 out of 104 hearts with the trifurcation pattern (97%), and 0 out of 2 hearts with the tetrafurcation pattern (0.0%). A significant relationship was detected between the incidence of the diagonal branches and the mode of branching of the LCA (Table 2) (Figs. 1,2,3).
The myocardial bridge was identified to obscure parts of the course of some branches of the LCA. Myocardial bridges were identified to obscure parts of the course of some branches of the LCA in 3 of 30 dissected cadaveric hearts. They were noticed to cross parts of the LAD and RI arteries. In CCTA, the myocardial bridges were observed in 27 of 200 scans (13.5%).
The myocardial bridges were observed in 30 out of 230 studied hearts (cadaver and CCTA only) (13.01%): 21 out of 168 hearts (12.5%) in the bifurcation pattern and 9 out of 59 hearts (15.2%) in the trifurcation pattern and 0 out of 2 hearts (0.0%) in the tetrafurcation pattern. The myocardial bridge could not be seen in the coronary catheterization. A significant relationship was detected between the incidence of these bridges and the mode of branching of the LCA (Table 3) (Figs. 1, 2).
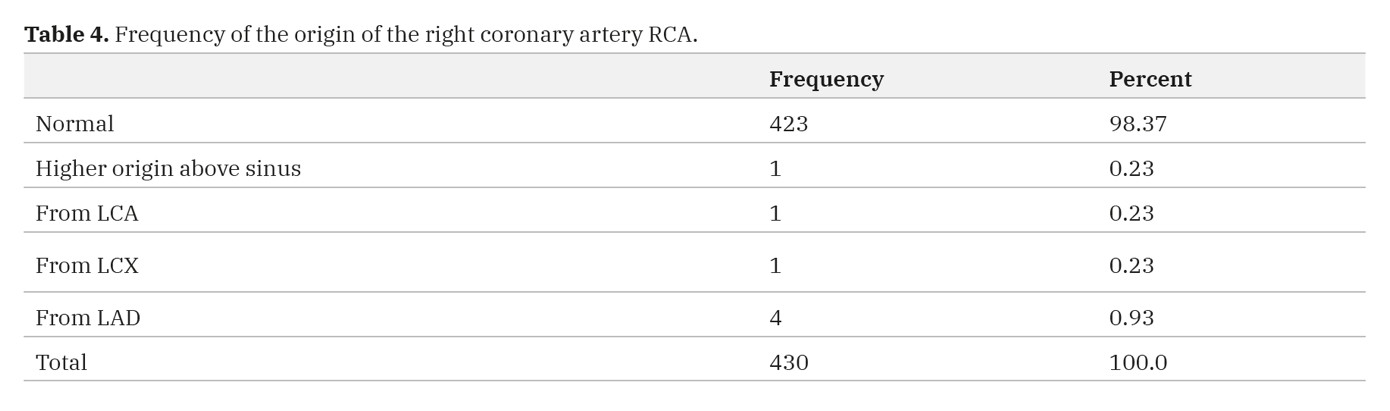
In the present study, the right coronary artery (RCA) showed abnormal origin from LCA and its branches as fellow: from LCA in 0.23% (1 case), from LCX in 0.23% (1 case), and from LAD in 0.93% (4 cases) (Table 4) (Fig. 3).
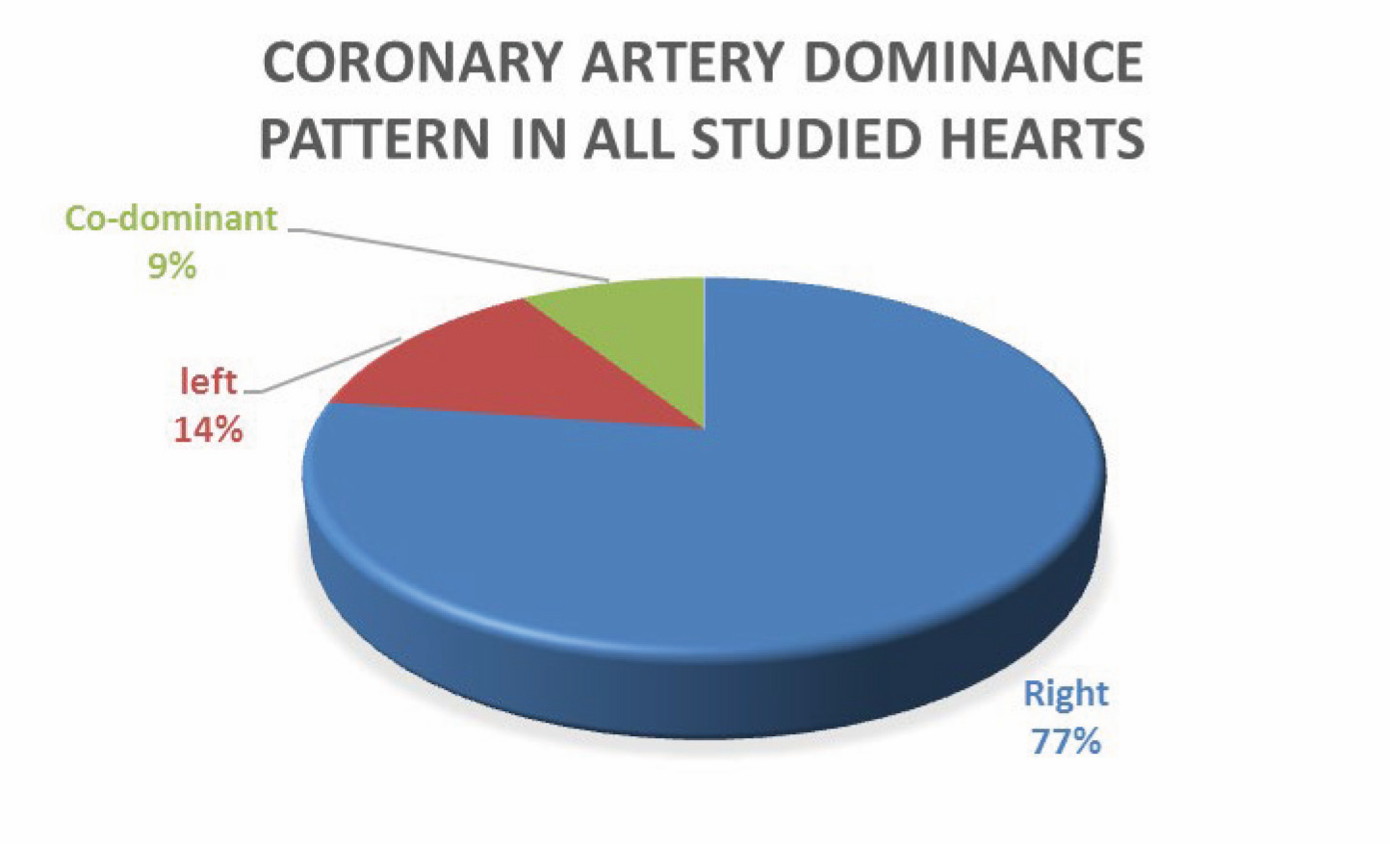
According to coronary circulation, the posterior descending (PD) artery arose from RCA in 77%. These were called ‘right dominant’. And PDA arose from LCX in 14% of studied hearts called ‘left dominant’ and in 9% both arteries gave origin to PDA. These were called ‘balanced type’ or ‘co-dominant’ (Figs. 4, 5).
DISCUSSION
Cardiovascular diseases are the leading cause of mortality worldwide, being responsible for about one-third of all deaths. With the increasing load of coronary heart diseases, the detailed anatomy of coronary arteries has been investigated by medical professionals (Tomar et al., 2013).
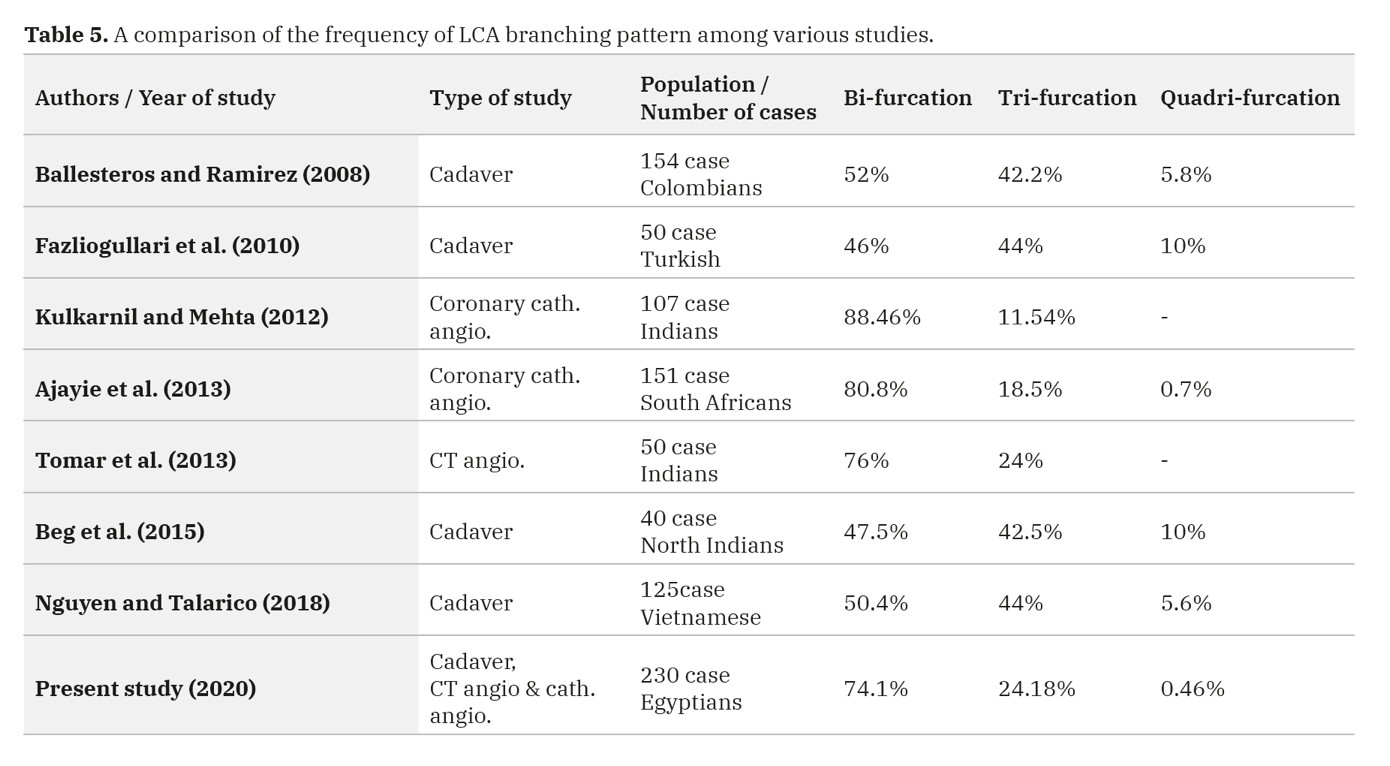
30 postmortem hearts, 200 3D CCTA scans, and 200 catheterization angiographies were enrolled in the present study to investigate the different patterns of the mode of branching of the left coronary artery. The current work has revealed that, in most of the specimens (99.07%), the LCA has arisen from the left posterior aortic sinus of the ascending aorta. This finding runs with what is reported by most authors (Kulkarnil and Metha, 2012; Dombe et al., 2012; Erol et al., 2013). The location and level of the coronary ostia are essential for the successful performance of a coronary angiogram (Taylor et al., 2000). In the present study, the LCA has been observed to run between the pulmonary trunk and left atrial appendage in all cases. This is coincident with most of the studies met within the literature (Cademartiri et al., 2008; Jacobs, 2010). The left coronary artery has been frequently mentioned to exhibit variations regarding the mode of its branching; it might be bifurcated, trifurcated, tetrafurcated or even pentafurcated (Ajayi et al., 2013). In the current investigation, the incidence of patterns of branching mode of the left coronary artery in all studied hearts (dissected and scanned), was 74.1% (bifurcated), 24.18% (trifurcated), and 0.46% (tetrafurcated). The incidences of the branching pattern of LCA reported in several large-scale studies are summarized in Table 5.
In the present work, the frequency of the bifurcation pattern of the LCA is more than threefold that of the trifurcation pattern (74.1% vs 24.18%). This is in agreement with Tomar et al. (2013), who mentioned that the incidence of the trifurcation pattern was about one-third that of the bifurcation pattern (24% vs 76%). Fazliogullari et al. (2010) reported a nearly equal incidence of both bifurcation and trifurcation patterns. The contradiction between these reported results and ours could be explained on grounds of the different approaches used for defining the ramus intermedius (RI) artery of the LCA.
Some authors consider the RI as an artery located in the angle between the LAD and CX arteries (Reig and Petit, 2004). Other authors considered that the RI artery as that originated from the vertex of the angle between LAD and CX arteries or from the initial millimeters of the LAD or CX artery themselves (Angelini et al., 1999). The present study has followed the way of identification of the RI artery that was mentioned by Reig and Petit. (2004).
The ramus intermedius (RI) artery represents an essential source of collateral blood flow in coronary insufficiency (Surucu et al., 2004; Shammas et al., 2009). The trifurcation of the LCA usually has no adverse hemodynamic effects and may play a protective role against the development of myocardial ischemia (Abuchaim et al., 2009). However, this pattern could cause technical difficulties in catheterization and might be a source of complication or misdiagnosis (Shammas et al., 2007; Koşar et al., 2009).
In the present study, a significant correlation between the incidence of the diagonal branches of the LAD artery and the branching patterns of LCA. Similar findings were reported by Reig and Petit. (2004)
In all the studies the majority of hearts were right dominant. Even though right dominance is predominant, the LCA is almost always considered more important than the RCA, as it is the major source of blood flow to the left ventricle in almost all humans even in those with anatomical right dominance.
The left dominance has been found to have significantly higher mortality than the right dominance and mixed dominance types (Goldberg et al., 2007). Dominance also plays an important role in the inferior wall infarcts of the heart. Inferior wall infarcts, although less extensive than anterior wall infarcts, are more important as they can cause various degrees of atrioventricular blocks in approximately 30% of cases (Agrawal and Arya, 2016).
In the present study, the incidence of left coronary dominance was assessed to be 13.5% of all hearts studied. Our left-dominant incidence is nearly similar to that reported by Fazliogullari et al. (2010) 14%. This incidence, herein, is lower than that reported by Ortale et al. (2005) who found that left coronary dominance is 25%.
In the present study, myocardial bridges are found across some of the branches of the LCA in 30 out of the 230 hearts. The current work has revealed a statistically significant relationship between the furcation pattern of LCA and the myocardial bridges. These results tally with the studies made by Loukas et al. (2006) and Beg et al. (2015).
Myocardial bridges may compress the coronary vessel underneath and compromise myocardial blood supply. Cases of sudden cardiac death where myocardial bridging is the only postmortem finding have been reported (Saidi et al., 2010).
The present investigation has demonstrated variations in the origin and branching pattern of the LCA. These variations could have anatomical, pathophysiological, diagnostic, and therapeutic implications. Moreover, before coronary revascularization procedures, precise evaluation and description of the coronary artery tree is greatly needed, in order to report possible coronary variations or anomalies which may cause technical difficulties during coronary interventional procedures and end in catastrophic complications for the patient.
Conclusions
A detailed study of LCA would be of use to cardiologists and interventional radiologists to predefine the abnormalities by invasive and non-invasive studies. Knowledge of individual and racial variations in coronary arteries is essential for the diagnosis and treatment of coronary artery patients. This morphological study may be helpful for interventional cardiologists and radiologists in diagnosis and in avoiding vascular trauma during diagnostic and therapeutic procedures.
ACKNOWLEDGEMENTS
The authors wish to thank Mohamed Gebreel, M.D. of radiology, who helps us in understanding the C.T coronary angiography. We are also grateful to Khaled Hussein, Msc of cardiology for his valuable guidance in reading the cardiac catheterizations.
Related articles
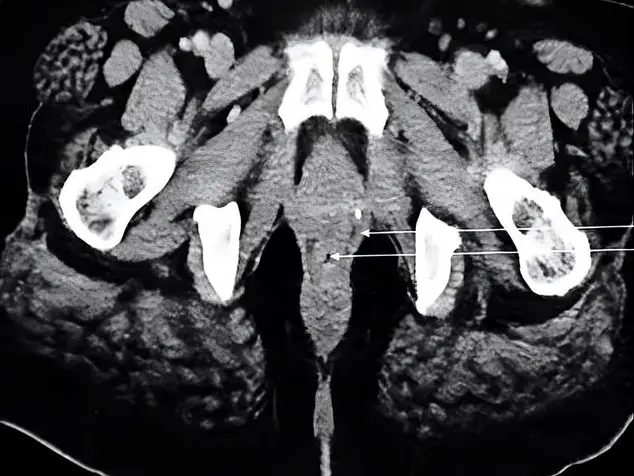
 Fig. 1.- A dissected human heart. A: bifurcation pattern of the left coronary artery (LCA) into the left anterior descending (LAD) and circumflex (CX) arteries. The LAD artery gives a diagonal (D) branch and the CX gives an obtuse marginal (OM) branch. Note: AO is referred to as ascending aorta and NA is referred to as a sinoatrial nodal branch of the left coronary artery. B: trifurcation pattern of the left coronary artery (LCA) into the left anterior descending artery (LAD), one ramus intermedius (RI), and circumflex artery (CX) branches. The RI artery appears equal in size to the LAD and gives muscular branches (M) to the left ventricle. C: left coronary artery (LCA) dividing into four branches (tetrafurcation): left anterior descending (LAD), circumflex (CX) and two ramus intermedius (RI) arteries. D: left coronary artery (LCA) dividing into two branches: left anterior descending (LAD) and circumflex (CX). Myocardial bridge (M.B.) interrupting the course of LAD is also observed.
Fig. 1.- A dissected human heart. A: bifurcation pattern of the left coronary artery (LCA) into the left anterior descending (LAD) and circumflex (CX) arteries. The LAD artery gives a diagonal (D) branch and the CX gives an obtuse marginal (OM) branch. Note: AO is referred to as ascending aorta and NA is referred to as a sinoatrial nodal branch of the left coronary artery. B: trifurcation pattern of the left coronary artery (LCA) into the left anterior descending artery (LAD), one ramus intermedius (RI), and circumflex artery (CX) branches. The RI artery appears equal in size to the LAD and gives muscular branches (M) to the left ventricle. C: left coronary artery (LCA) dividing into four branches (tetrafurcation): left anterior descending (LAD), circumflex (CX) and two ramus intermedius (RI) arteries. D: left coronary artery (LCA) dividing into two branches: left anterior descending (LAD) and circumflex (CX). Myocardial bridge (M.B.) interrupting the course of LAD is also observed.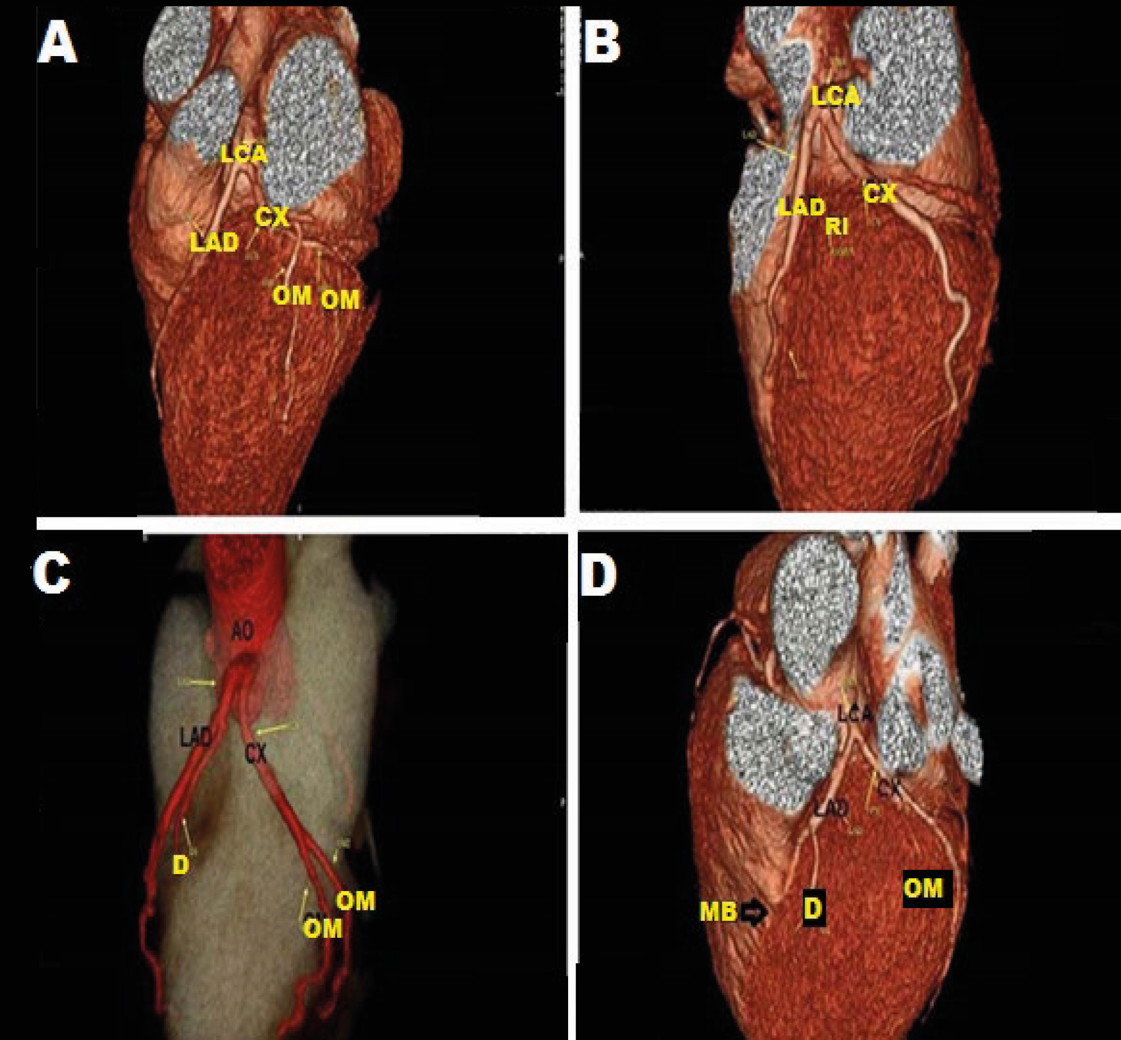 Fig. 2.- 3D CT coronary angiography. A: The left coronary artery (LCA) dividing into left anterior descending (LAD) and circumflex (CX) arteries. Two obtuse marginal (OM) arteries are branches of CX. B: The left coronary artery (LCA) dividing into left anterior descending (LAD) and circumflex (CX) arteries. A diagonal branch (D) is seen arisen from LAD and obtuse marginal (OM) is seen arise from CX. C: The left anterior descending (LAD) and circumflex (CX) arteries are arising directly from the ascending aorta (AO) by a separate ostium and the left coronary artery (LCA) is absent. A diagonal branch (D) is seen arisen from LAD and obtuse marginal (OM) is seen arise from CX. D: The left coronary artery (LCA) dividing into left anterior descending (LAD) and circumflex (CX) arteries. A diagonal branch (D) is seen arisen from LAD and obtuse marginal (OM) is seen arise from CX. Myocardial bridge (M.B.) interrupting the course of LAD is also observed.
Fig. 2.- 3D CT coronary angiography. A: The left coronary artery (LCA) dividing into left anterior descending (LAD) and circumflex (CX) arteries. Two obtuse marginal (OM) arteries are branches of CX. B: The left coronary artery (LCA) dividing into left anterior descending (LAD) and circumflex (CX) arteries. A diagonal branch (D) is seen arisen from LAD and obtuse marginal (OM) is seen arise from CX. C: The left anterior descending (LAD) and circumflex (CX) arteries are arising directly from the ascending aorta (AO) by a separate ostium and the left coronary artery (LCA) is absent. A diagonal branch (D) is seen arisen from LAD and obtuse marginal (OM) is seen arise from CX. D: The left coronary artery (LCA) dividing into left anterior descending (LAD) and circumflex (CX) arteries. A diagonal branch (D) is seen arisen from LAD and obtuse marginal (OM) is seen arise from CX. Myocardial bridge (M.B.) interrupting the course of LAD is also observed.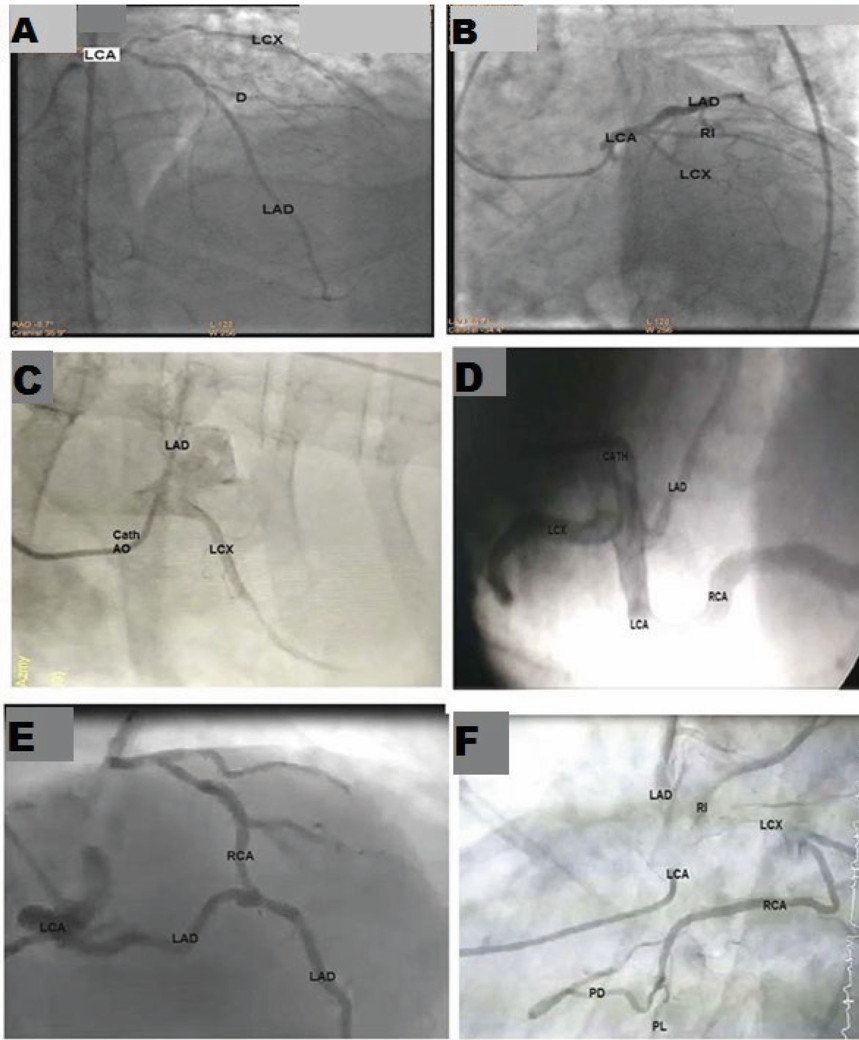 Fig. 3.- Coronary catheterization angiography study showing: A: The left coronary artery (LCA) dividing into left anterior descending (LAD) and circumflex (LCX) arteries (bifurcation). One diagonal (D) is seen as a branch of LAD. B: The left coronary artery (LCA) dividing into 3 branches: left anterior descending (LAD), circumflex (LCX), and ramus intermedius (RI) arteries (Trifurcation). C: Absent left coronary artery (LCA). As left anterior descending (LAD) and left circumflex (LCX) arteries arise from separate ostium from the aorta. D: The left coronary artery (LCA) is dividing into left anterior descending (LAD) and left circumflex (LCX) arteries and also gives rise to the right coronary artery (RCA) from its beginning. E: The left coronary artery (LCA) is dividing into left anterior descending (LAD) and left circumflex (LCX) arteries. The right coronary artery (RCA) is raised from LAD. F: The left coronary artery (LCA) is dividing into left anterior descending (LAD), left circumflex (LCX), and ramus intermedius (RI) arteries. RCA is raised from LCX. RCA is terminated into two terminal branches (PL and PD).
Fig. 3.- Coronary catheterization angiography study showing: A: The left coronary artery (LCA) dividing into left anterior descending (LAD) and circumflex (LCX) arteries (bifurcation). One diagonal (D) is seen as a branch of LAD. B: The left coronary artery (LCA) dividing into 3 branches: left anterior descending (LAD), circumflex (LCX), and ramus intermedius (RI) arteries (Trifurcation). C: Absent left coronary artery (LCA). As left anterior descending (LAD) and left circumflex (LCX) arteries arise from separate ostium from the aorta. D: The left coronary artery (LCA) is dividing into left anterior descending (LAD) and left circumflex (LCX) arteries and also gives rise to the right coronary artery (RCA) from its beginning. E: The left coronary artery (LCA) is dividing into left anterior descending (LAD) and left circumflex (LCX) arteries. The right coronary artery (RCA) is raised from LAD. F: The left coronary artery (LCA) is dividing into left anterior descending (LAD), left circumflex (LCX), and ramus intermedius (RI) arteries. RCA is raised from LCX. RCA is terminated into two terminal branches (PL and PD).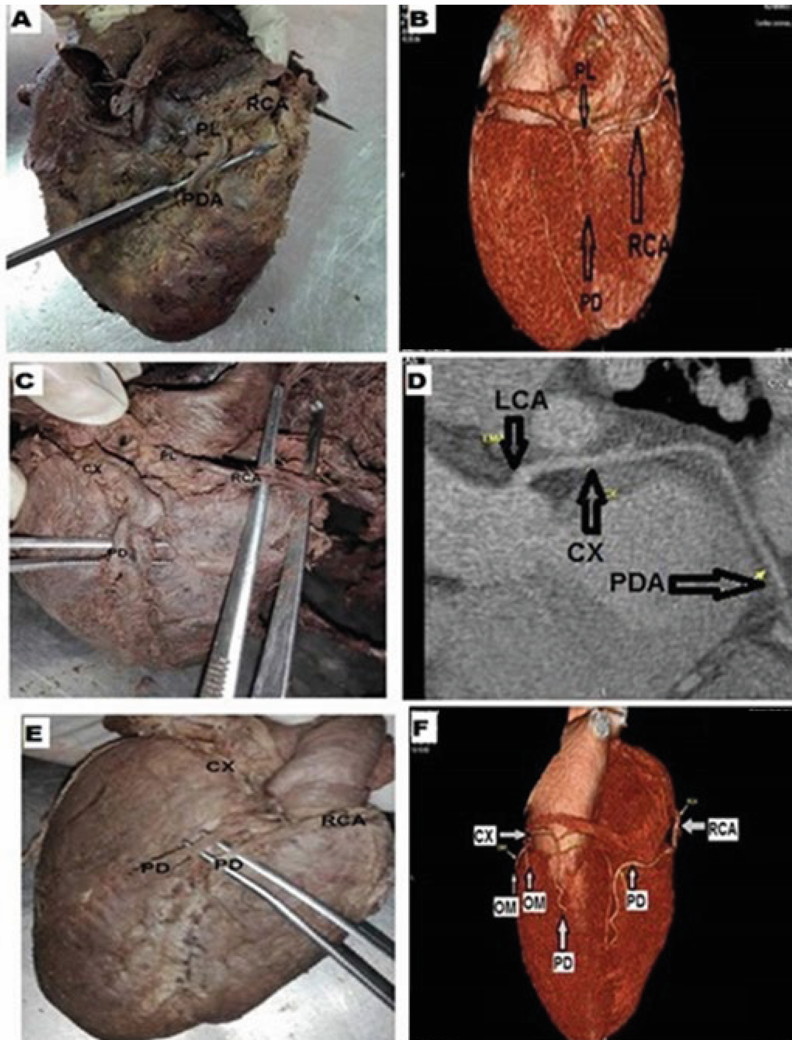 Fig. 4.- Pictures of A: Cadaver dissection and B: 3D CT angiography. Both of them showing the right coronary artery (RCA) termination into a posterior descending artery (PDA) and posterolateral artery (PL) in the right dominant heart. C: Cadaver dissection and D: 3D CT angiography showing a left dominance pattern where the posterior descending artery (PD) arose from the circumflex artery (CX), not from the right coronary artery (RCA). RCA is terminated by giving the posterolateral artery (PL). E: Cadaver dissection and F: 3D CT angiography showing a balanced pattern where the posterior descending artery (PD) arises from both the right coronary artery (RCA) and circumflex artery (CX), and both PD lying within the posterior interventricular sulcus.
Fig. 4.- Pictures of A: Cadaver dissection and B: 3D CT angiography. Both of them showing the right coronary artery (RCA) termination into a posterior descending artery (PDA) and posterolateral artery (PL) in the right dominant heart. C: Cadaver dissection and D: 3D CT angiography showing a left dominance pattern where the posterior descending artery (PD) arose from the circumflex artery (CX), not from the right coronary artery (RCA). RCA is terminated by giving the posterolateral artery (PL). E: Cadaver dissection and F: 3D CT angiography showing a balanced pattern where the posterior descending artery (PD) arises from both the right coronary artery (RCA) and circumflex artery (CX), and both PD lying within the posterior interventricular sulcus.ABUCHAIM DCS, SPERA CA, FARACO DL, FILHO JMR, MALAFAIA O (2009) Coronary dominance patterns in the human heart investigated by corrosion casting. Revista Brasileira de Cirurgia Cardiovascular, 24(4): 514-518.
AGRAWAL R, ARYA RS (2016) Anatomical study of coronary dominance and variations of posterior interventricular artery in cadaveric human heart. Int J Sci Res, 5(3): 531-534.
AJAYI NO, LAZARUS L, VANKER EA, SATYAPAL KS (2013) Anatomic parameters of the left coronary artery: an angiographic study in a South African population. Int J Morphol, 31(4): 1393-1398.
ALTIN C, KANYILMAZ S, KOC S, GURSOY YC, BAL U, AYDINALP A, YILDIRIR A, MUDERRISOGLU H (2015) Coronary anatomy, anatomic variations and anomalies: a retrospective coronary angiography study. Singapore Med J, 56(6): 339-345.
ANGELINI P, VILLASON S, CHAN AV, DIEZ JG (1999) Normal and anomalous coronary arteries in humans. In: Angelini P (ed). Coronary artery anomalies. A comprehensive approach. Lippincot Williams & Wilkins, Philadelphia, pp 27-79.
BALLESTEROS LE, RAMIREZ LM (2008) Morphological expression of the left coronary artery: a direct anatomical study. Folia Morphol, 67(2): 135-142.
BEG MRU, SINGH A, GOEL S, GOEL AK, GOEL V, GOYAL P, SURANA A, SINGH NK, DHANDA MS (2015) Anatomical variations of coronary artery and frequency of median artery: A cadaveric study from Northern India. Int Arch Integ Med IAIM, 2(5): 88-94.
CADEMARTIRI F, LA GRUTTA LL, MALAGÒ R, ALBERGHINA F, MEIJBOOM WB, PUGLIESE F, MAFFEI E, PALUMBO AA, ALDROVANDI A, FUSARO M, BRAMBILLA V, CORUZZI P, MIDIRI M, MOLLET NRA, KRESTIN GP (2008) Prevalence of anatomical variants and coronary anomalies in 543 consecutive patients studied with 64-slice CT coronary angiography. Eur Radiol, 18(4): 781-791.
CHOUGULE P, SILOTRY N, CHAVAN L (2014) Variation in branching pattern of coronary arteries. Int J Sci Res, 3(8): 270-273.
DAS H, DAS G, DAS DC, TALUKDAR K (2010) A study of coronary arterial dominance in the population of Assam. J Anat Soc India, 59(2): 187-191.
DOMBE DD, ANITHA T, GIRI PA, DOMBE SD, AMBIYE MV (2012: Clinically relevant morphometric analysis of left coronary artery. Int J Biol Med Res, 3(1): 1327-1330.
EROL C, KOPLAY M, PAKSOY Y (2013) Evaluation of anatomy, variation and anomalies of the coronary arteries with coronary computed tomography angiography. Anatolian J Cardiol, 13(2): 154-164.
FAZLIOGULLARI Z, KARABULUT AK, DOGAN NU, UYSAL II (2010) Coronary artery variations and median artery in Turkish cadaver hearts. Singapore Med J, 51(10): 775-780.
FISS DM (2007) Normal coronary anatomy and anatomic variations. App Radiol, 36: 14-26.
GOLDBERG A, SOUTHERN D, GALBRAITH PD, TRABOULSI M, KNUDTSON ML, GHALI WA (2007) Coronary dominance and prognosis of patients with acute coronary syndrome. Am Heart J, 154(6): 1116-1122.
GRAIDIS C, DIMITRIADIS D, KARASAVVIDIS V, DIMITRIADIS G, ARGYROPOULOU E, ECONOMOU F, GEORGE D, ANTONIOU A, KARAKOSTAS G (2015) Prevalence and characteristics of coronary artery anomalies in an adult population undergoing multi-detector row computed tomography for the evaluation of coronary artery disease. BMC Cardiovasc Disorders, 15(1(: 112.
JACOBS JE (2010) Computed tomographic evaluation of the normal cardiac anatomy. Radiol Clinics North Am, 48(3): 701-710.
KINI S, BIS KG, WEAVER L (2007) Normal and variant coronary arterial and venous anatomy on high-resolution CT angiography. AJR Am J Roentgenol, 188(6): 1665-1674.
KOSAR P, ERGUN E, OZTURK C, KOSAR U (2009) Anatomic variations and anomalies of the coronary arteries: 64slice CT angiographic appearance. Diagnostic Intervent Radiol, 15(4): 275-283.
KULKARNIL JP, MEHTA L (2012) Main left coronary artery system – angiographic anatomy. IOSR J Dental Med Sci, 3(2): 5-7.
LOUKAS M, CURRY B, BOWERS M, LOUIS RG, BARTCZAK A, KIEDROWSKI M, KAMIONEK M, FUDALEJ M, WAGNER T (2006) The relationship of myocardial bridges to coronary artery dominance in the adult human heart. J Anat, 209(1): 43-50.
LOZANO R (2012) Global and regional mortality from 235 causes of death for 20 age groups in 1990 and 2010: a systematic analysis for the Global Burden of Disease Study 2010. Lancet, 380(9859): 2095-2128.
MOORE K, DALLEY AF (2006) Clinically Oriented Anatomy. Lippincott Williams & Wilkins, Baltimore, Chapter 5, pp 9-156.
NGUYEN VH, TALARICO JR EF (2018) A morphometric anatomical study on the division of the left main coronary artery and myocardial bridges. Eur J Anat, 22 (4): 355-365.
ORTALE JR, FILHO JM, PACCOLA AMF, LEAL JG, SCARANARI CA (2005) Anatomy of the lateral, diagonal and anterosuperior arterial branches of the left ventricle of the human heart. Brazilian J Cardiovasc Surg, 20(2): 149-158.
REIG J, PETIT M (2004) Main trunk of the left coronary artery: anatomic study of the parameters of clinical interest. Clin Anat, 17(1): 6-13.
ROY S, GUPTA A, NANRAH BK, VERMA M, SAHA R (2014) Morphometric study of left coronary artery trunk in adult human cadavers: a study on the eastern region population anatomy section. J Clin Diagnost Res, 8(2): 7-9.
SAIDI H, ONGETI WK, OGENG’O J (2010) Morphology of human myocardial bridges and association with coronary artery disease. African Health Sci, 10(3): 242-247.
SHAMMAS NW, DIPPEL EJ, AVILA A, GEHBAUER L, FARLAND L, BROSIUS S, JERIN M, WINTER M, STOAKES P, BYRD J, MAJETIC L, SHAMMAS G, SHARIS P, ROBKEN J (2007) Long-term outcomes in treating left main trifurcation coronary artery disease with the Paclitaxel-Eluting stent. J Invasive Cardiol, 19(2): 77-82.
SHAMMAS NW, SHAMMAS GA, JERIN M, PARIKH A, COIN K, DIPPEL E, SHARIS P, ROBKEN J (2009) Treatment of left main coronary trifurcation lesions with the Paclitaxel drug-Eluting stent: mid-term outcomes from a tertiary medical center. J Invasive Cardiol, 21(7): 321-325.
SNELL RS (2011) Clinical anatomy by regions. Lippincott Williams and Wilkins, Chapter 3, pp 86-87.
SURUCU HS, KARAHAN ST, TANYELI E (2004): Branching pattern of the left coronary artery and an important branch. The median artery. Saudi Medical Journal; 25(2):177-81.
TAKEUCHI S, IMAMURA H, KATSUMOTO K, HAYASHI I, KATOHGI T, YOZU R, OHKURA M, INOUE T (1979) New surgical method for repair of anomalous left coronary artery from pulmonary artery. J Thoracic Cardiovasc Surg, 78(1): 7-11.
TAYLOR AM, THORNE SA, RUBENS MB, JHOOTI P, KEEGAN J, GATEHOUSE PD, WIESMANN F, GROTHUES F, SOMERVILLE J, PENNELL DJ (2000) Coronary artery imaging in grown up congenital heart disease complementary role of magnetic resonance and X-ray coronary angiography. Circulation, 101(14): 1670-1678.
TOMAR S, AGA P, SHARMA PK, MANIK P, SRIVASTAVA AK (2013) Normal and variant anatomy of left coronary artery: 64-multi detector computed tomography (MDCT) coronary angiographic depiction in North Indian population. Int J Sci Res, 3(8): 1-17.
WANG SP, JAO YT, HAN SC (2008) Acute coronary syndrome due to high aortocoronary junction of the right coronary artery: the value of multislice CT. Int J Cardiol, 123: 59-61.
YOUNG PM, GERBER TC, WILLIAMSON EE, JULSRUD PR, HERFKENS RJ (2011) Cardiac imaging: Part 2, normal, variant and anomalous configurations of the coronary vasculature. AJR Am J Roentgenol, 197(4): 816-826.